Minimizing HAPIs from NIPPV
Vapotherm Clinical Nurse Educator
The views and ideas presented in this blog article are solely those of the author, and the content is not intended to serve as medical advice. Vapotherm does not practice medicine or provide medical services. Practitioners should refer to the full indications for use and operating instructions of any products referenced herein before prescribing them.
UlcerTraining/Default.aspxRead Full Text Initial and ongoing education on pressure injury prevention and management should exist for both nursing and non-nursing staff.1010. Agency for Healthcare Quality and Research (AHRQ).Pressure ulcer toolkit. 2014.https://www.ahrq.gov/professionals/systems/hospital/pressureulcertoolkit/putool7b.htmlRead Full Text
UlcerTraining/Default.aspxRead Full Text
4. Haesler, E. Pressure injuries: Preventing medical device related pressure injuries. Wound Practice & Research. 2017; 25(4): 214-216 Removal of the device as soon as medically feasible is critical to minimizing the skin damage.11. National Pressure Ulcer Advisory Panel (NPUAP), European Pressure Ulcer Advisory Panel (EPUAP) and Pan Pacific Pressure Injury Alliance (PPPIA). Prevention and treatment of pressure ulcers: Quick reference guide. Emily Haesler (Ed.). Cambridge Media: Osborne Park, Australia; 2014. Retrieved from http://www.npuap.org/wp-content/uploads/2014/08/Quick-Reference-Guide-DIGITAL-NPUAP-EPUAP-PPPIA-Jan2016.pdfRead Full Text
UlcerTraining/Default.aspxRead Full Text
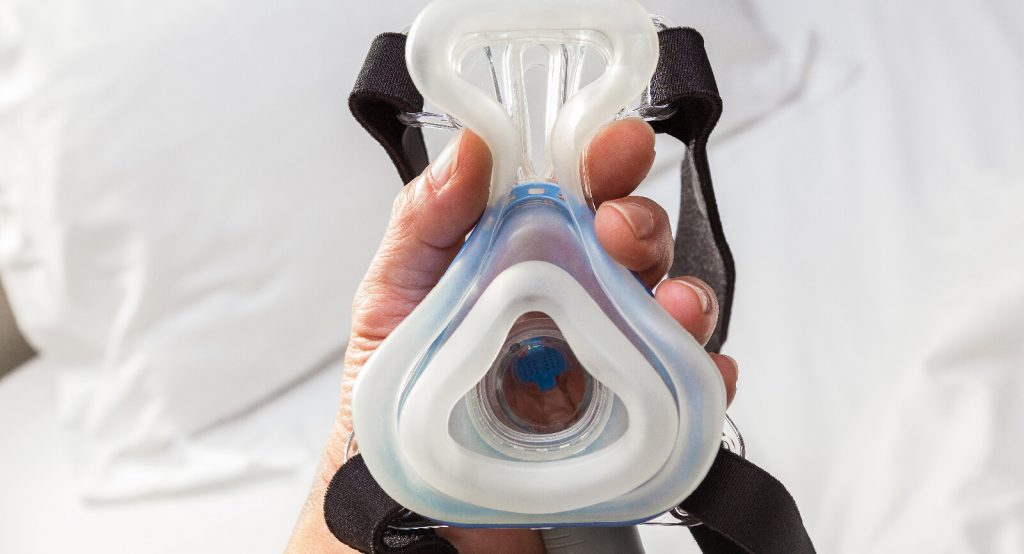
- Follow proper mask or interface selection and fit techniques—assess for skin risk factors
- Apply facility approved cushioning to points of mask-skin contact: forehead, nasal bridge, below nares or nasal septum.
- Skin assessment under and around interface device at least two times a day—document skin assessment
- Moisture management practices—keep skin clean and dry
- Rotate interface type and placement
- Remove mask when medically feasible. Proceed to step #1.
6. Yamaguti W, Moderno E, Yamashita S, Gomes T, Maida A, Kondo C, de Salles I, de Brito C. Treatment-related risk factors for development of skin breakdown in patients with acute respiratory failure undergoing noninvasive ventilation or CPAP. Respiratory Care 2014; 59(10): 1-7Read Full Text To identify patient risk for skin breakdown, it is recommended to use a risk assessment tool that is appropriate to the population, is valid and reliable.11. National Pressure Ulcer Advisory Panel (NPUAP), European Pressure Ulcer Advisory Panel (EPUAP) and Pan Pacific Pressure Injury Alliance (PPPIA). Prevention and treatment of pressure ulcers: Quick reference guide. Emily Haesler (Ed.). Cambridge Media: Osborne Park, Australia; 2014. Retrieved from http://www.npuap.org/wp-content/uploads/2014/08/Quick-Reference-Guide-DIGITAL-NPUAP-EPUAP-PPPIA-Jan2016.pdfRead Full Text The Braden Scale is widely used for the adult patient population and the Braden Q Scale for the pediatric patient population. The scale consists of six subscales and the total scores range from 6-23. A lower Braden score indicates higher levels of risk for pressure ulcer development. Generally, a score of 18 or less indicates at-risk status.1111. Braden B & Bergstrom N. The Braden Scale for predicating pressure sore risk. 1998; http://www.bradenscale.com/images/bradenscale.pdfRead Full Text The risk assessment tool is used in conjunction with clinical assessment to determine patients at risk for pressure injury and provide for early intervention and care planning. Abnormal scores in the individual subscales should be addressed accordingly.
7. Nava S, Navalesi P, & Gregoretti, C. Interfaces and humidification for noninvasive mechanical ventilation. Respiratory Care 2009; 54(1)Read Full Text Many options exist for mask selection requiring skilled decision making and careful attention to individual patient needs. According to Visscher et al, few interface options are available to offset pressure. The mask fit method, however, is used to select masks from available options, to identify the potential areas of increased tissue pressure, and to prevent skin injury.55. Visscher MO,White CC, Jones JM, Cahill T, Jones DC, Pan BS. Face masks for noninvasive ventilation: Fit, excess skin hydration, and pressure ulcers. Respiratory Care 2015; 60(11): 1536-1547.Read Full Text Avoiding an excessively tight fitting interface was found to be the most important strategy to prevent pressure injury.77. Nava S, Navalesi P, & Gregoretti, C. Interfaces and humidification for noninvasive mechanical ventilation. Respiratory Care 2009; 54(1)Read Full Text To ensure enough space exists between the mask and the skin, it is recommended that 2 fingers can pass beneath the headgear.77. Nava S, Navalesi P, & Gregoretti, C. Interfaces and humidification for noninvasive mechanical ventilation. Respiratory Care 2009; 54(1)Read Full Text The small amount of air leak that may occur is acceptable and should not affect the interaction between the patient and ventilation mode.77. Nava S, Navalesi P, & Gregoretti, C. Interfaces and humidification for noninvasive mechanical ventilation. Respiratory Care 2009; 54(1)Read Full Text
Figure 1: Examples of hydrophilic soft silicone foam to mask-skin contact areas (adapted from CNMC)
4. Haesler, E. Pressure injuries: Preventing medical device related pressure injuries. Wound Practice & Research. 2017; 25(4): 214-216 Many options exist for mask selection requiring skilled decision making and careful attention to individual patient needs. According to Visscher et al, few interface options are available to offset pressure. The mask fit method, however, is used to select masks from available options, to identify the potential areas of increased tissue pressure, and to prevent skin injury.55. Visscher MO,White CC, Jones JM, Cahill T, Jones DC, Pan BS. Face masks for noninvasive ventilation: Fit, excess skin hydration, and pressure ulcers. Respiratory Care 2015; 60(11): 1536-1547.Read Full Text Avoiding an excessively tight fitting interface was found to be the most important strategy to prevent pressure injury.77. Nava S, Navalesi P, & Gregoretti, C. Interfaces and humidification for noninvasive mechanical ventilation. Respiratory Care 2009; 54(1)Read Full Text Individuals with evidence of localized edema should be assessed more often than twice a day to detect first signs of injury.44. Haesler, E. Pressure injuries: Preventing medical device related pressure injuries. Wound Practice & Research. 2017; 25(4): 214-216 It is important to note that monitoring frequency is based upon patient relative risk and should be performed accordingly using clinical judgment and institutional guidelines for optimal prevention strategy implementation.
References
1. National Pressure Ulcer Advisory Panel (NPUAP), European Pressure Ulcer Advisory Panel (EPUAP) and Pan Pacific Pressure Injury Alliance (PPPIA). Prevention and treatment of pressure ulcers: Quick reference guide. Emily Haesler (Ed.). Cambridge Media: Osborne Park, Australia; 2014. Retrieved from http://www.npuap.org/wp-content/uploads/2014/08/Quick-Reference-Guide-DIGITAL-NPUAP-EPUAP-PPPIA-Jan2016.pdf
2. Agency for Healthcare Quality and Research (AHRQ), Preventing pressure injuries in hospitals, a toolkit for improving quality of care. 2017;Retrieved from www.ahrq.gov
3. National Database of Nursing Quality Indicators (NDNQI). Medical Device Related (MDR) Pressure Injuries. Retrieved from https://members.nursingquality.org/NDNQIPressureUlcerTraining/Default.aspx
4. Haesler, E. Pressure injuries: Preventing medical device related pressure injuries. Wound Practice & Research. 2017; 25(4): 214-216
5. Visscher MO,White CC, Jones JM, Cahill T, Jones DC, Pan BS. Face masks for noninvasive ventilation: Fit, excess skin hydration, and pressure ulcers. Respiratory Care 2015; 60(11): 1536-1547.
6. Yamaguti W, Moderno E, Yamashita S, Gomes T, Maida A, Kondo C, de Salles I, de Brito C. Treatment-related risk factors for development of skin breakdown in patients with acute respiratory failure undergoing noninvasive ventilation or CPAP. Respiratory Care 2014; 59(10): 1-7
7. Nava S, Navalesi P, & Gregoretti, C. Interfaces and humidification for noninvasive mechanical ventilation. Respiratory Care 2009; 54(1)
8. Kiss E, Heiler, M. Pediatric skin integrity practice guideline for institutional use: A quality improvement project. Journal of Pediatric Nursing 2014; 29(4): 362-367
9. Newnam KM, McGrath JM, Salyer J, Estes T Jallo , Bass WT. A comparative effectiveness study of continuous positive airway pressure-related skin breakdown when using different nasal interfaces in the extremely low birth weight neonate. Applied Nursing Research 2015. 28; 36-41
10. Agency for Healthcare Quality and Research (AHRQ).Pressure ulcer toolkit. 2014.https://www.ahrq.gov/professionals/systems/hospital/pressureulcertoolkit/putool7b.html
11. Braden B & Bergstrom N. The Braden Scale for predicating pressure sore risk. 1998; http://www.bradenscale.com/images/bradenscale.pdf
12. Children’s National Medical Center (CNMC). Nursing practice guideline for skin care 2017.
This webpage contains links to third party abstracts and/or publications. With respect to those materials, please note that Vapotherm’s Hi-VNI® technology is a tool for treating the signs and symptoms of respiratory distress in patients for whom prescribers desire to add heat and moisture to breathing gases. The linked materials may describe certain outcomes in relation to the use of Vapotherm’s Hi-VNI Technology, but individual results may vary. Practitioners should refer to the full indications for use and operating instructions of any products referenced herein before prescribing them.
[fusion_modal name=”study-5″ title=”Face masks for noninvasive ventilation: Fit, excess skin hydration, and pressure ulcers.” size=”large” background=”” show_footer=”no”]
[/fusion_modal]
[fusion_modal name=”study-6″ title=”Treatment-related risk factors for development of skin breakdown in patients with acute respiratory failure undergoing noninvasive ventilation or CPAP.” size=”large” background=”” show_footer=”no”]
[/fusion_modal]
[fusion_modal name=”study-7″ title=”Interfaces and humidification for noninvasive mechanical ventilation.” size=”large” background=”” show_footer=”no”]
[/fusion_modal]
[fusion_modal name=”study-8″ title=”Pediatric skin integrity practice guideline for institutional use: A quality improvement project.” size=”large” background=”” show_footer=”no”]
[/fusion_modal]
[fusion_modal name=”study-9″ title=”A comparative effectiveness study of continuous positive airway pressure-related skin breakdown when using different nasal interfaces in the extremely low birth weight neonate.” size=”large” background=”” show_footer=”no”]
[/fusion_modal]
[fusion_modal name=”study-11″ title=”The Braden Scale for predicating pressure sore risk.” size=”large” background=”” show_footer=”no”]
[/fusion_modal]